If you or someone you love is living with type 1 diabetes, there’s one emergency medication that should always be part of the conversation: glucagon.
This life-saving medicine is something I find myself discussing often in clinic—especially after seeing several patients with type 1 diabetes in one day. It’s the kind of medication you hope you never need, but one you absolutely want to have on hand in the event of a severe low blood sugar emergency.
What Is Glucagon?
Glucagon is a hormone-based medication used to raise blood sugar levels rapidly when someone is experiencing severe hypoglycemia—typically defined as a blood glucose less than 54 mg/dL—and is:
- Unconscious,
- Having a seizure,
- Unable to eat or drink safely, or
- Not responding to usual methods of glucose intake.
In these situations, it may not be possible to treat a low blood sugar with food or juice. That’s where glucagon becomes essential—it stimulates the liver to release stored glucose into the bloodstream, quickly increasing blood sugar levels.
Types of Glucagon Available
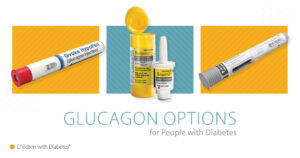
Fortunately, glucagon is now available in several user-friendly forms:
- Nasal spray (e.g., Baqsimi): No needles, easy to administer.
- Autoinjector pens (e.g., Gvoke HypoPen): Similar in design to an EpiPen.
- Traditional syringe and vial kits: Effective but require mixing before use.
The newer delivery methods have made it much easier for caregivers, friends, and family to administer glucagon in high-stress situations. This is a major improvement from the days when the only option required mixing powder with liquid and injecting it quickly during a medical emergency.
When Might Glucagon Be Needed?
Glucagon is used in critical moments, such as:
- Loss of consciousness from low blood sugar
- Seizures caused by hypoglycemia
- Inability to keep food or glucose down due to nausea or vomiting
- Persistent low blood sugar that isn’t responding to typical treatments (like juice, glucose tabs, or fast-acting carbs)
While it’s not something to be used casually—it can be expensive—it’s a lifesaving tool when the usual strategies fail.
What You Can Do
- Talk to your healthcare provider about keeping a glucagon prescription on file.
- Check the expiration date on your glucagon and replace it as needed.
- Educate those around you—spouse, partner, child’s teacher, coach, roommate—on when and how to use it.
- Keep it accessible: in your home, your bag, or with your diabetes supplies.
Final Thoughts
Glucagon is one of the most important tools in preventing tragedy from severe hypoglycemia. If you’re on insulin, particularly with type 1 diabetes, I strongly encourage you to take this part of your diabetes emergency plan seriously.
You may never need it—but if you do, having it can make all the difference.